In the wellness landscape of 2026, the obsession with restrictive dieting has been superseded by a more sophisticated physiological objective: Metabolic Flexibility. This term describes the body’s ability to efficiently switch between different fuel sources—primarily glucose (carbohydrates) and fatty acids (stored body fat)—based on availability and demand. In an era of constant caloric abundance, most modern humans have lost this innate evolutionary capacity, becoming “sugar burners” who are metabolically locked into carbohydrate dependency. Restoring this flexibility is now recognized as the fundamental prerequisite for sustained energy, cognitive clarity, and long-term weight management.
The technical essence of metabolic flexibility lies in the mitochondrial switch. When the body is metabolically inflexible, the mitochondria (the power plants of the cell) lose the enzymatic machinery required to oxidize fat effectively. This leads to the “mid-afternoon crash,” systemic inflammation, and the inability to access stored adipose tissue even in a caloric deficit. By 2026, clinical protocols have shifted from “counting calories” to “training the metabolism,” utilizing specific nutritional and lifestyle interventions to upregulate the pathways responsible for lipid oxidation, thereby turning the human body into a dual-fuel engine.
Achieving this state does not require radical biohacking or futuristic genetic editing; it requires a return to biological basics informed by modern data. Metabolic flexibility provides a buffer against the metabolic syndrome and type 2 diabetes by ensuring that insulin levels remain optimized and that the body can maintain stable blood glucose levels without the need for constant exogenous fuel. For the high-performing individual in 2026, metabolic flexibility is the “operating system” upon which all other wellness interventions—from sleep to strength training—are built.
The Mitochondria as an Energy Sensor: The Role of PGC-1alpha
At the cellular level, metabolic flexibility is governed by a master regulator known as PGC-1alpha (Peroxisome proliferator-activated receptor gamma coactivator 1-alpha). This protein acts as an energy sensor that coordinates mitochondrial biogenesis—the creation of new mitochondria—and improves the efficiency of existing ones. When PGC-1alpha is active, the cell is more capable of switching from glucose to fatty acid oxidation. In 2026, the focus of metabolic health has narrowed down to this specific pathway, utilizing strategies like hormetic stress (cold exposure, heat, and exercise) to trigger its expression.
The efficiency of this “switch” is also dependent on the concentration of carnitine palmitoyltransferase 1 (CPT1), the enzyme responsible for transporting fatty acids into the mitochondria for burning. A metabolically inflexible individual often has high levels of malonyl-CoA, which inhibits CPT1 and effectively “locks” the fat in the cells. By manipulating these biochemical levers through strategic fasting and movement, we can lower malonyl-CoA and “unlock” the fat-burning machinery, leading to a state of metabolic efficiency that feels like a constant, steady stream of energy rather than a series of spikes and crashes.
Metabolic flexibility is not just about what you eat, but about the body’s competence in processing what you’ve already stored.
Nutrient Timing and the 2026 Approach to Insulin Sensitivity
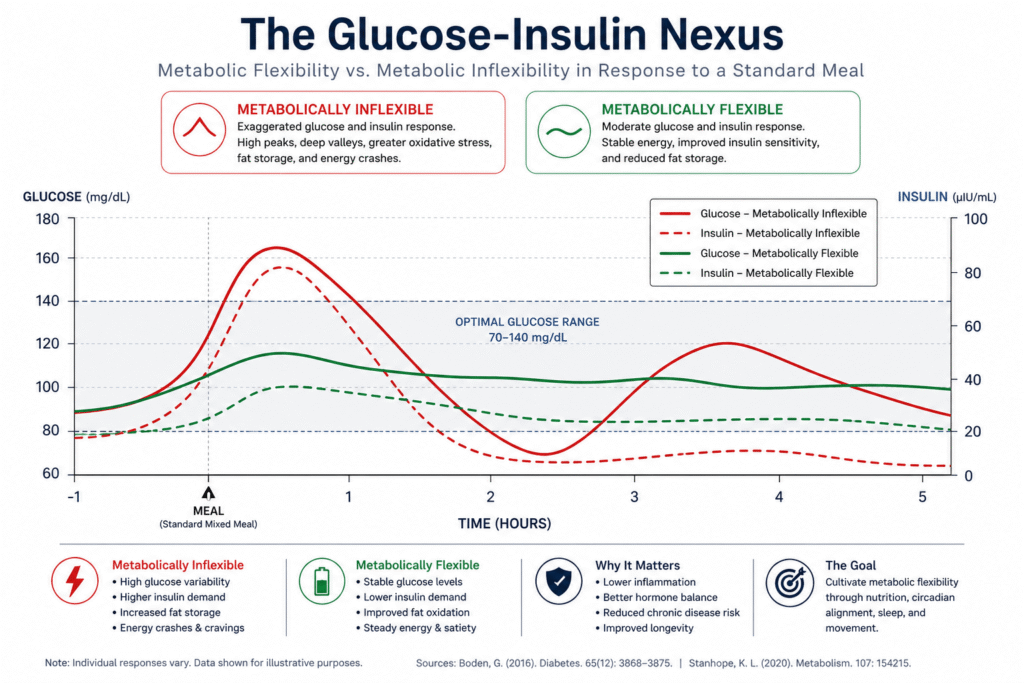
The primary obstacle to metabolic flexibility is chronic hyperinsulinemia—constantly high levels of insulin caused by frequent snacking and high-carbohydrate intake. Insulin is an anabolic, storage-focused hormone; when it is elevated, the body is biologically prevented from accessing stored fat. In 2026, the strategic use of Nutrient Timing is the most effective way to lower the “insulin floor.” By concentrating carbohydrate intake around periods of high physical activity, we ensure that glucose is shuttled into the muscles via non-insulin-dependent pathways (GLUT4 translocation), leaving the rest of the day for fat oxidation.
This approach is best visualized by the stability of blood glucose throughout the day. A metabolically flexible person experiences minor, controlled undulations in glucose, whereas an inflexible person experiences volatile spikes followed by hypoglycemic dips that drive hunger and fatigue. The following table compares the two primary fuel sources and their impact on the 2026 metabolic profile:
| Feature | Glucose Oxidation (Carbs) | Fatty Acid Oxidation (Fat) | Metabolic Impact |
| ATP Yield | Low per molecule | Very High per molecule | Efficiency |
| Storage Capacity | Limited (Glycogen) | Virtually Unlimited | Endurance |
| Insulin Response | High | Negligible | Fat Loss |
| Byproducts | More Reactive Oxygen Species | Lower Oxidative Stress | Longevity |
By 2026, the “Standard American Diet” of six small meals a day has been debunked as a recipe for metabolic rigidity. Instead, Intermittent Fasting or “Time-Restricted Feeding” has become the standard for restoring insulin sensitivity. These periods of caloric absence force the body to rely on its internal stores, “dusting off” the enzymatic pathways for fat burning that would otherwise remain dormant.
Low-Intensity Steady State and the Optimization of Fat Oxidation
While high-intensity training has its place, the most effective tool for building the metabolic base in 2026 is Zone 2 Training or Low-Intensity Steady State (LISS). This is the intensity level where the body is most efficient at burning fat as its primary fuel source. At higher intensities, the body is forced to switch back to glucose because fat oxidation is a slower, oxygen-dependent process. By spending time in Zone 2, we specifically train the mitochondrial density in slow-twitch muscle fibers, increasing the “Fat Max”—the maximum rate at which an individual can oxidize fat.
In the 2026 wellness paradigm, Zone 2 training is viewed as “aerobic base building.” It is the foundation that allows an individual to handle higher-intensity stressors without crashing. For a professional, this translates to better stress resilience and the ability to maintain focus for hours without needing a “glucose hit.” This type of movement—brisk walking, light cycling, or swimming—is accessible, low-impact, and arguably the most important physical intervention for reversing metabolic inflexibility.
Digital Biomarkers: Using Continuous Glucose Monitors for Metabolic Auditing
The rise of the “quantified self” in 2026 has made metabolic health visible in real-time. Continuous Glucose Monitors (CGM), once reserved for diabetics, are now standard equipment for wellness enthusiasts. A CGM provides a 24/7 view of how specific foods, sleep quality, and stress levels impact blood sugar. This data allows for “Metabolic Auditing,” where individuals can identify exactly which “healthy” foods are causing exaggerated glucose spikes that stall their fat-burning capacity.
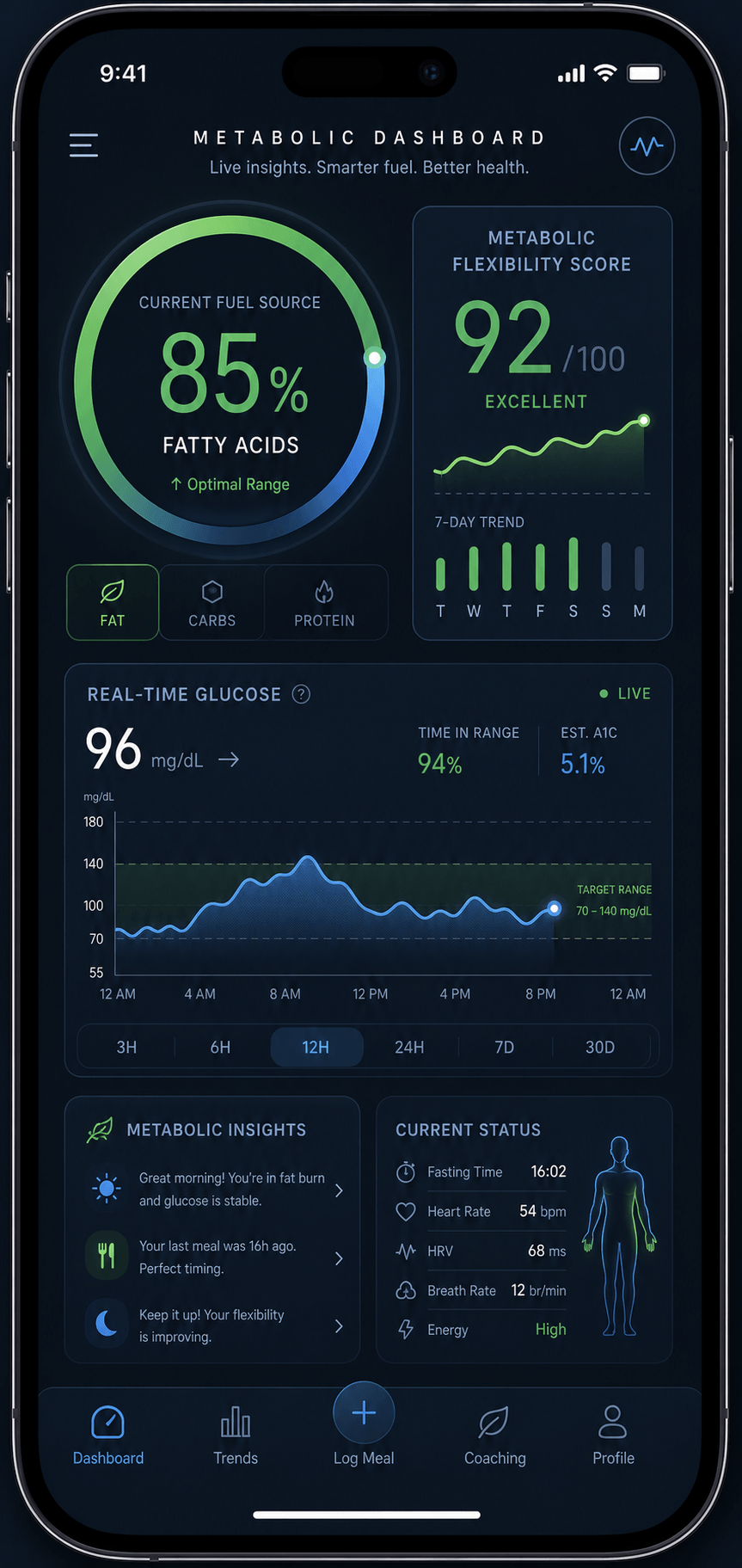
By 2026, AI-driven apps integrate CGM data with activity trackers to provide a Metabolic Flexibility Score. This score tells the user when their body is in a “fat-burning state” and when it is “sugar-dependent.” This real-time feedback loop is more powerful than any generic diet plan, as it accounts for individual bio-individuality. For example, two people can eat the same apple and have vastly different glucose responses; the CGM identifies these nuances, allowing for a truly personalized metabolic strategy.
To begin the journey toward metabolic flexibility, follow this Metabolic Reset Checklist:
- Extend the Overnight Fast: Start with a 12-hour window and gradually move to 14 or 16 hours.
- Prioritize Protein and Fiber: Both have a negligible impact on insulin compared to refined carbs.
- Earn Your Carbs: Save high-glycemic foods for the post-workout window when muscles are “sponges” for glucose.
- Walk After Meals: A 10-minute walk significantly blunts the glucose spike of a meal.
- Audit Your Sleep: Poor sleep (less than 7 hours) dramatically increases insulin resistance the following day.
FAQ: Human Metabolism and Energy Optimization
Can I be metabolically flexible while following a vegan or vegetarian diet?
Yes. Metabolic flexibility is about the body’s capability, not a specific food group. While animal proteins are often more “metabolically neutral” regarding insulin, a well-planned plant-based diet rich in fiber, healthy fats (avocados, nuts), and fermented foods can absolutely support a flexible metabolism. The key is avoiding the “processed vegan” trap of refined grains and sugars which drive insulin resistance regardless of the source.
How long does it take to “restore” metabolic flexibility if I’ve been a sugar-burner for years?
The initial enzymatic adaptations usually take 2 to 4 weeks of consistent intervention (fasting and Zone 2). However, full mitochondrial “remodeling” can take 3 to 6 months. Most people notice a significant shift in hunger levels and mental clarity within the first 14 days as the body begins to access its “fat tank” more reliably.
Does caffeine help or hurt metabolic flexibility in 2026?
Caffeine is a double-edged sword. It stimulates lipolysis (the breakdown of fat into the bloodstream), which can provide raw fuel for oxidation. However, in a stressed individual, caffeine can also trigger a cortisol spike, which in turn causes the liver to dump glucose into the blood, potentially stalling fat burning. The 2026 recommendation is to consume caffeine in a “fed” state or alongside movement to ensure the liberated fatty acids are actually burned.
Why is sleep so closely linked to my ability to burn fat?
Sleep deprivation is a massive metabolic disruptor. Just one night of 4-5 hours of sleep can create a state of temporary insulin resistance equivalent to that of a pre-diabetic. This happens because lack of sleep elevates cortisol and ghrelin (the hunger hormone) while suppressing leptin (the fullness hormone), making it biologically impossible for the “mitochondrial switch” to function correctly the next day.