The Health Savings Account (HSA) has evolved into the most potent tax-advantaged vehicle within the United States financial system as of 2026. Often misunderstood as a mere “spending account” for immediate medical needs, the HSA offers a unique Triple Tax Advantage that surpasses traditional 401(k) and IRA structures in pure fiscal efficiency. Contributions are 100% tax-deductible (or pre-tax via payroll), investment earnings grow entirely tax-free, and withdrawals for qualified medical expenses incur no federal or state tax liability. For the sophisticated beneficiary, the HSA functions as a “stealth IRA” that provides an essential hedge against the rising costs of healthcare in retirement.
In the current 2026 regulatory environment, the IRS has adjusted the parameters for HSA eligibility to account for inflationary pressures on the broader economy. Unlike Flexible Spending Accounts (FSAs), which generally operate on a “use-it-or-lose-it” basis, HSA funds are fully portable and remain with the individual regardless of job changes or retirement. This permanence allows for long-term compound growth, turning a health-focused account into a cornerstone of a diversified wealth management strategy. However, maintaining this status requires strict adherence to the qualifying health plan mandates and the avoidance of “prohibited transactions” that could trigger account disqualification.
The strategic deployment of an HSA in 2026 involves more than just hitting the contribution ceiling; it requires a deep understanding of the coordination of benefits and the specific timing of expense reimbursements. Many high-net-worth individuals are now adopting the “investor mindset,” paying for current out-of-pocket medical costs with post-tax dollars while allowing their HSA balance to remain invested in equities and index funds. This approach maximizes the tax-free compounding period, essentially creating a dedicated, tax-free fund specifically earmarked for the six-figure healthcare expenses typical of the late-life stage.
The HDHP Prerequisite and Minimum Deductible Thresholds
To be eligible to contribute to an HSA in 2026, an individual must be covered by a High Deductible Health Plan (HDHP) and have no other “disqualifying coverage,” such as a general-purpose Health FSA or Medicare. For the 2026 plan year, the IRS has increased the minimum annual deductible for an HDHP to $1,700 for self-only coverage and $3,400 for family coverage. It is critical to note that an HDHP must generally not provide any benefits—other than preventive care—until the minimum deductible is met.
The definition of preventive care has seen subtle expansions in 2026, allowing certain chronic condition treatments (such as insulin or blood pressure monitoring) to be covered before the deductible is satisfied without disqualifying the HSA. However, the Maximum Out-of-Pocket (MOOP) limits have also risen, now capped at $8,500 for individuals and $17,000 for families. This ceiling includes all deductibles, co-payments, and co-insurance, but specifically excludes monthly insurance premiums. Navigating these thresholds requires a careful balance between premium savings and the potential for high immediate costs.
The most common compliance failure in 2026 occurs when individuals enroll in a spouse’s non-HDHP plan or a traditional “Medical FSA,” which provides first-dollar coverage and immediately nullifies their legal right to contribute to an HSA.
Failure to remain an “eligible individual” for the entire year can result in the proration of your contribution limit. If you lose HDHP coverage mid-year, you must adjust your contributions to reflect only the months you were eligible as of the first day of the month. This calculation is essential to avoid the 6% excise tax on excess contributions, a penalty that applies annually for as long as the over-contribution remains in the account.
2026 Contribution Limits and the “Last-Month Rule” Nuances
The IRS has announced significantly higher contribution ceilings for 2026 to help taxpayers offset rising medical inflation. These limits apply to the combined total of employer and employee contributions. For those looking to maximize their tax savings, the following table details the shifts in the 2026 regulatory landscape compared to the previous year:
| Contribution Category | 2025 Limit | 2026 Limit | Net Change |
| Self-Only Coverage | $4,300 | $4,400 | +$100 |
| Family Coverage (2+) | $8,550 | $8,750 | +$200 |
| Catch-up (Age 55+) | $1,000 | $1,000 | No Change |
The “Last-Month Rule” provides a technical “safe harbor” for those who become eligible late in the year. If you are an eligible individual on December 1, 2026, the IRS allows you to contribute the full annual maximum for that year, regardless of how many months you were actually enrolled. However, this benefit comes with a mandatory “Testing Period”: you must remain HSA-eligible through December 31, 2027. If you fail this period for any reason other than death or disability, the “extra” contributions become taxable income and are subject to an additional 10% penalty tax.
Strategic Reimbursement: The “Shoebox” Method for Long-Term Growth
A sophisticated strategy gaining traction in 2026 is the “Shoebox Method,” which leverages the fact that there is no IRS-mandated deadline for when you must reimburse yourself for a medical expense. As long as the expense was incurred after the HSA was established, you can hold onto the receipt and withdraw the funds years, or even decades, later. This effectively allows the money that would have been used for reimbursement to remain in the market, benefiting from tax-free compound interest.
To execute this properly, a taxpayer must maintain a “forensic” digital record of all qualified medical expenses. In 2026, specialized fintech apps allow users to scan receipts and link them to their HSA provider’s database without actually initiating a withdrawal. This creates a “latent” pool of tax-free liquidity that can be tapped during a financial emergency or in retirement to supplement income without increasing your Adjusted Gross Income (AGI). This lack of a “statute of limitations” on reimbursements is one of the most powerful, yet underutilized, loopholes in the tax code.
Furthermore, the definition of “qualified” has expanded to include many over-the-counter (OTC) medications and menstrual care products without a prescription. However, one must distinguish between “medical care” and “general health”. Expenses for items like vitamins or gym memberships typically require a specific Letter of Medical Necessity (LMN) from a physician to qualify for tax-free distribution. Maintaining this LMN in your “shoebox” is vital for surviving an IRS audit of your distributions.
Portability, Beneficiary Designations, and Post-65 Distributions
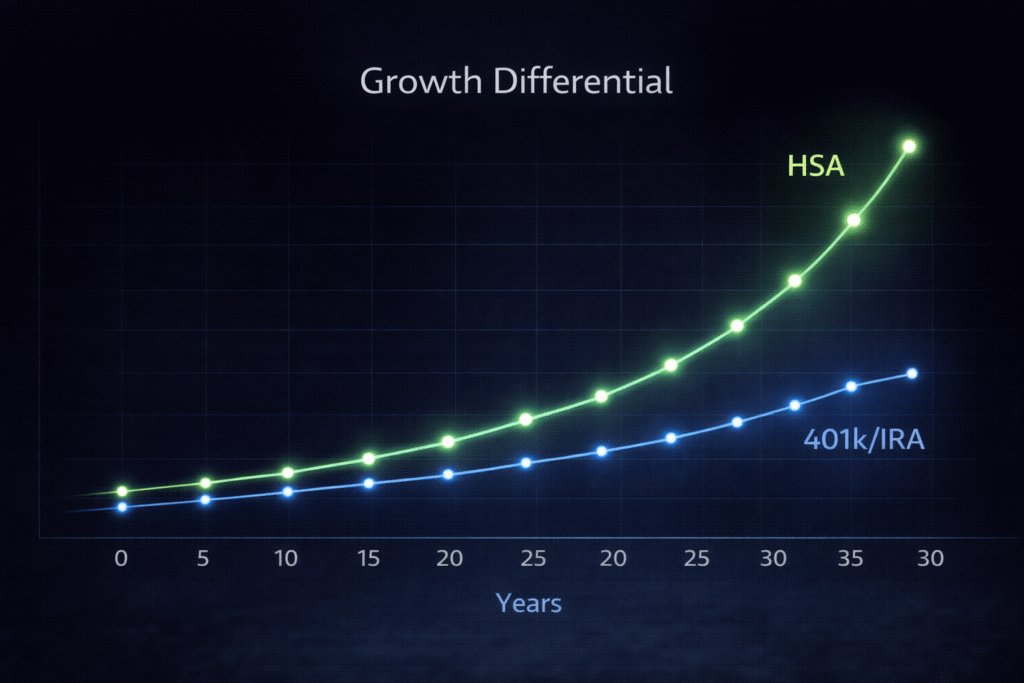
Once you reach age 65, the HSA undergoes a functional transformation. While you can no longer contribute to the account once enrolled in Medicare Part A or B, you can continue to use the existing funds for any purpose. If used for non-medical expenses after 65, the 20% penalty is waived, and the withdrawal is simply taxed as ordinary income—effectively making it identical to a Traditional IRA. However, if used for qualified medical expenses, it remains 100% tax-free, which still gives it the edge over retirement accounts that are always taxed upon distribution.
Correctly managing Beneficiary Designations is a technical necessity for estate planning. If a spouse is the beneficiary, the HSA remains an HSA after the owner’s death, retaining all tax advantages. However, if the beneficiary is a non-spouse (like a child or a trust), the account ceases to be an HSA on the date of death and the fair market value becomes fully taxable to the beneficiary in that year. This “tax bomb” makes the HSA a “spend-first” asset for those without a surviving spouse.
The list of qualified medical expenses for 2026 is extensive but requires precise categorization to avoid penalties. Key items include:
- Professional Services: Dental cleanings, orthodontic care, and vision exams (including LASIK).
- Medications: Both prescription drugs and many OTC items like pain relievers and allergy meds.
- Long-Term Care: Premiums for qualified long-term care insurance (subject to age-based IRS limits).
- Medicare Premiums: After age 65, HSA funds can pay for Medicare Part B and Part D premiums.
- Mental Health: Therapy, psychiatric care, and prescribed smoking cessation programs.
FAQ: Health Savings Accounts and IRS Compliance
How does the 2026 “Catch-up” contribution work for spouses who are both over age 55?
If both spouses are 55 or older and covered under a family HDHP, they can both contribute an additional $1,000 catch-up. However, unlike the standard contribution, the $1,000 catch-up cannot be “pooled” into a single HSA. Each spouse must have their own individual HSA account to receive their respective $1,000 catch-up. If you put $2,000 into one spouse’s account, $1,000 will be considered an excess contribution.
Can I use my 2026 HSA funds to pay for medical expenses incurred by my 24-year-old child who is on my health plan?
This is a common technical trap. While the ACA allows children to stay on your health insurance until age 26, the Internal Revenue Code has a different definition for “tax dependents”. You can only use HSA funds for your child’s expenses if they qualify as a legal tax dependent on your tax return. If your 24-year-old is working and not a dependent, they cannot use your HSA, but they may actually be eligible to open their own individual HSA with the full family contribution limit ($8,750) if they are covered by your family HDHP.
What happens if I contribute the maximum for 2026 and then enroll in Medicare in July?
Your eligibility for the year would be prorated. Since you were eligible for only 6 months (January through June), you can only contribute 50% of the annual limit (e.g., $2,200 for self-only). If you contributed more, you must withdraw the excess and the earnings on that excess by the tax filing deadline in April 2027 to avoid the 6% excise tax.
Is there a limit on how many times I can roll over or transfer my HSA to a new provider?
There are two ways to move funds: a Trustee-to-Trustee Transfer and a Rollover. There is no limit on how many direct transfers you can perform; the money moves directly between institutions. However, if you take a check yourself (a Rollover), you are limited to one rollover every 12 months, and you must redeposit the funds into a new HSA within 60 days to avoid taxes and a 20% penalty.